Language and semantics can help or hinder relationships with study volunteers and advocacy leaders. Terminology and semantics will impact inference and intent and can absolutely affect the tone of the conversation. This module provides common terminology and tools on reframing language for more successful rapport.
CONCEPT
Members of the STARR Coalition represent a wide range of fields; pharma, CRO’s, clinical research, treatment, academia, advocacy, as such, many of our areas of expertise require very specific language. In the mental health arena, for example, language is especially important to those receiving services. Many individuals feel that as people living with psychiatric conditions, they have been marginalized by the industry and society in general. Language can be a contributor to those feelings. Over the years, the practice of person-centered or person-first language has emerged.
We recognize that in many cases it is appropriate to use specific language to designate the relationship of the individual to the provider of services. For instance, it is appropriate for a doctor to refer to the person they are serving as a “patient”. This is the norm in society. In the same vein it is important that people are not labeled by their diagnoses, people are not schizophrenics or bipolars, they are people living with schizophrenia or living with bipolar disorder.
Language should not be a barrier to achieving our goals. When appropriate it is acceptable to talk about patients, clients, and subjects as long as it is used in the appropriate environment. The point is that relationships between researchers and individuals participating in a study are better when we can accentuate personhood. In essence people are people first.
There is an expectation all stakeholders within The STARR to simply recognize language as a potential barrier and agree to never let semantics get in the way of meaning progress. Many times, we must remind those in different areas of work that the language we use is the language given to us.
COMMON TERMINOLOGY
Labels we give people living with different indications evolve over time. Terminology changes; such as mentally retarded, mentally deficient, feeble-minded, mentally handicapped to more recent terms like developmentally delayed, developmentally disabled, cognitively impaired. Many people will dismiss this as “political correctness”, but remember, it matters to the person being spoken to.
We also see the same dynamic in the labels we use for those participating in a trial. For instance:
• Within research: Subject, volunteer
• Within medical community: Patient
• Within treatment: Client, consumer
• Within advocacy: Person living with (indication), person with lived experience
Many times, if you use the term “subject” to an advocate, there could be a misunderstanding you only see the person as an experimental subject and not the as an individual. The reality is we use the language given to us in our specific area of expertise. Yet, we must know how our language can be interpreted by others who are not within your field. Instances have occurred where an advocate has heard a research describe someone as a “subject” and the advocate shut down the conversation. Simply acknowledging to others that you don’t wish language to be a barrier is a step in the right direction.
The following are terms used in the treatment realm. Many individuals entering a study will be familiar with these terms.
Assertive community treatment (ACT): a team approach to providing rehabilitation and support to individuals who require intensive services in order to live in the community
Caregiver: A person who has special training to help people with mental health problems. Examples include social workers, teachers, psychologists, psychiatrists, and mentors.
Case manager: An individual who organizes and coordinates services and supports for individuals with mental health problems and their families. (Alternate terms: service coordinator, advocate, and facilitator.)
Case management: A service that helps people arrange for appropriate services and supports. A case manager coordinates mental health, social work, educational, health, vocational, transportation, advocacy, respite care, and recreational services, as needed. The case manager makes sure that the changing needs of the individual served are met.
Continuum of care: A term that implies a progression of services that a individual moves through, usually one service at a time. More recently, it has come to mean comprehensive services. Also see system of care and wraparound services.
Crisis intervention training (CIT): a specialized law enforcement unit comprised of officers who have received training in how to interact with individuals experiencing a psychiatric crisis.
Cultural competence: Help that is sensitive and responsive to cultural differences. Caregivers are aware of the impact of culture and possess skills to help provide services that respond appropriately to a person’s unique cultural differences, including race and ethnicity, national origin, religion, age, gender, sexual orientation, or physical disability. They also adapt their skills to fit a family’s values and customs.
Day treatment: Day treatment includes special education, counseling, vocational training, skill building, crisis intervention, and recreational therapy. It lasts at least 4 hours a day. Day treatment programs work in conjunction with mental health, recreation, and education organizations and may even be provided by them.
Early intervention: A process used to recognize warning signs for mental health problems and to take early action against factors that put individuals at risk. Early intervention may help individuals get better in less time and can prevent problems from becoming worse.
Family support services: Help designed to keep the family together, while coping with mental health problems that affect them. These services may include consumer information workshops, in-home supports, family therapy, parenting training, crisis services, and respite care.
Individualized services: Services designed to meet the unique needs of each individual and family. Services are individualized when the caregivers pay attention to the needs and strengths, ages, and stages of development of the individual and family members.
Interdisciplinary team (IDT): a team approach to treatment; typically consists of a psychiatrist, a case manager, a nurse and a peer specialist (an individual whose mental illness is stable)
Plan of Care: A treatment plan especially designed for each individual and family, based on the individual’s strengths and needs. The caregiver(s) develop(s) the plan with input from the individual being served. The plan establishes goals and details appropriate treatment and services to meet the special needs of the individual.
Recovery: Recovery is the personal process that people with mental health conditions experience in gaining control, meaning and purpose in their lives.
Residential treatment centers: Facilities that provide treatment 24 hours a day. Individuals with serious mental illness may receive constant supervision and care. Treatment may include individual, group, and family therapy; behavior therapy; special education; recreation therapy; and medical services. Residential treatment is usually more long-term than inpatient hospitalization. Centers are also known as therapeutic group homes.
System of Care: A spectrum of effective, community-based services and supports for individuals with or at risk for mental health or other challenges and their families, that is organized into a coordinated network, builds meaningful partnerships with families and individuals while addressing their cultural and linguistic needs, in order to help them to function better at home, in school, in the community, and throughout life.
As times change, the words people prefer change. To show respect in conversations with others, be mindful of the impact your word choices have. If you need to use a descriptive term but are unsure of the words to use, ask the person how he or she would like to be addressed or referred to.
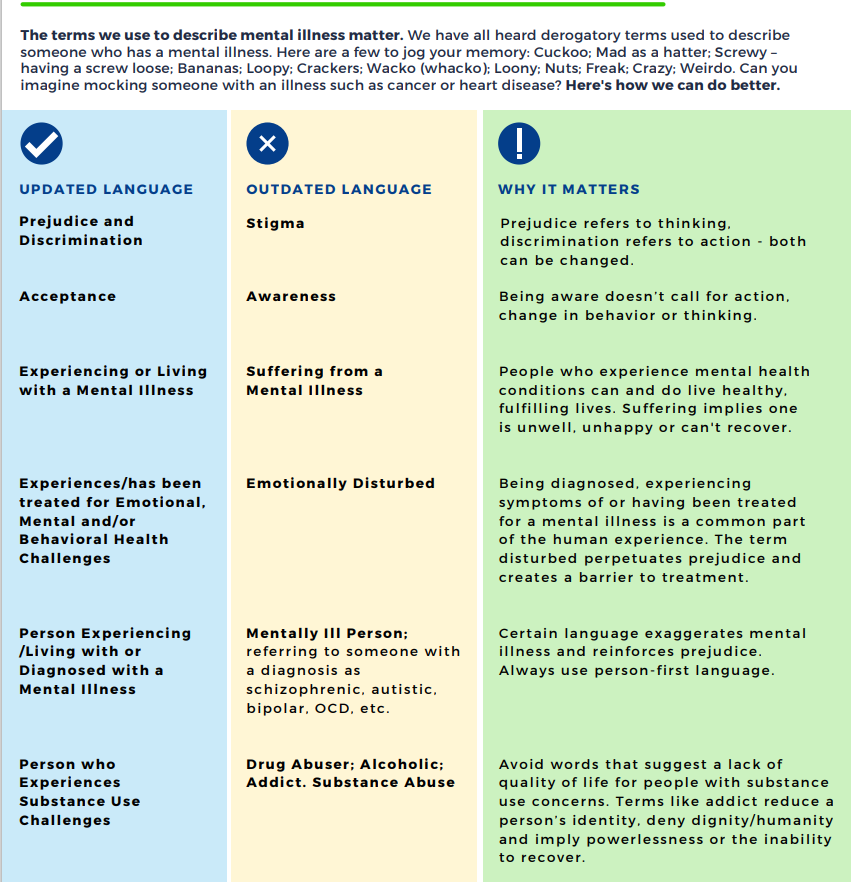
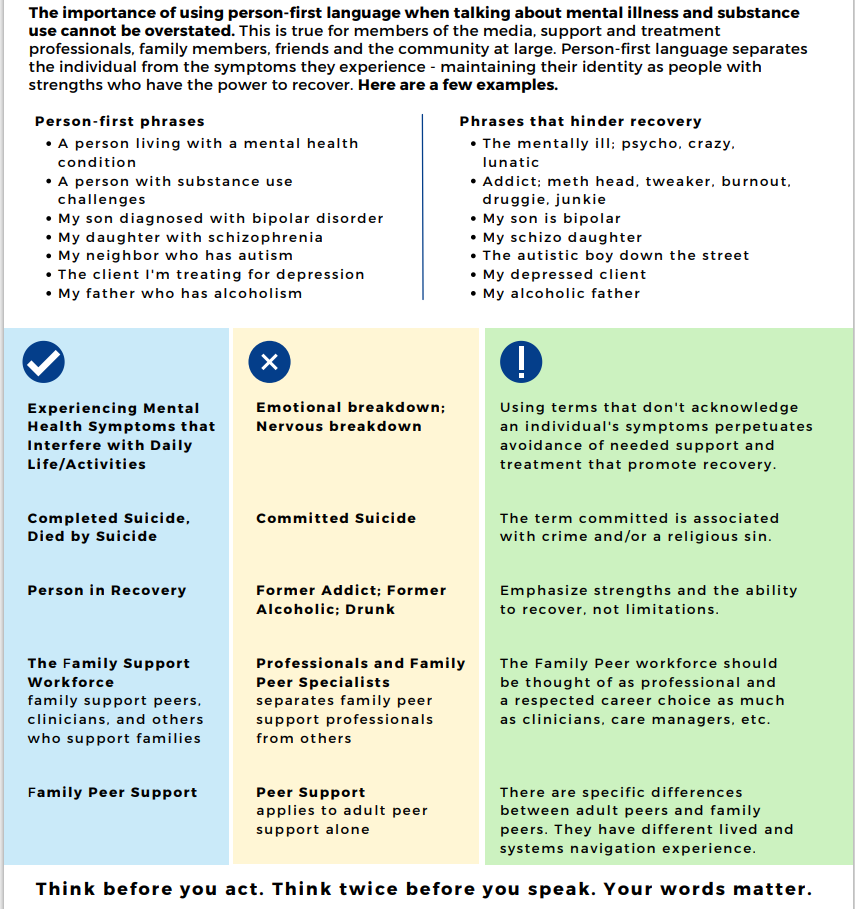
With thanks to the National Family Support and Technical Assistance Center, which developed this great infographic.
